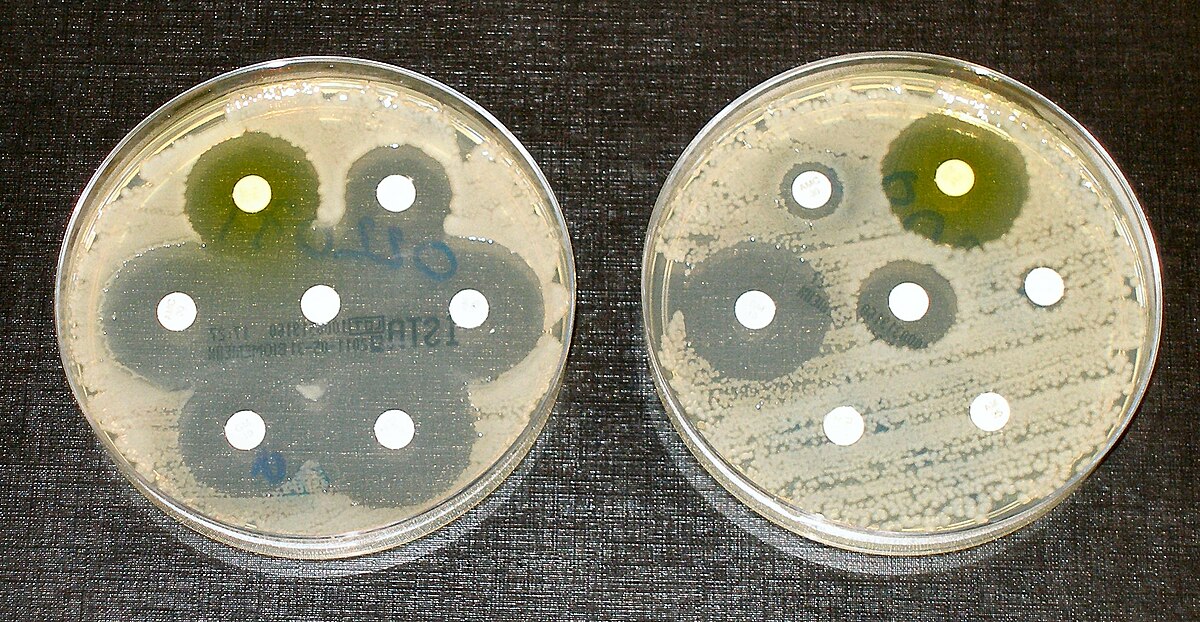
Antimicrobial resistance
Antimicrobial resistance (AMR or AR) occurs when microbes evolve mechanisms that protect them from antimicrobials, which are drugs used to treat infections.[ 2] This resistance affects all classes of microbes, including bacteria (antibiotic resistance), viruses (antiviral resistance), protozoa (antiprotozoal resistance), and fungi (antifungal resistance). Together, these adaptations fall under the AMR umbrella, posing significant challenges to healthcare worldwide.[ 3] Misuse and improper management of antimicrobials are primary drivers of this resistance, though it can also occur naturally through genetic mutations and the spread of resistant genes.[ 4]
Microbes resistant to multiple drugs are termed multidrug-resistant (MDR) and are sometimes called superbugs.[ 5] Antibiotic resistance, a significant AMR subset, enables bacteria to survive antibiotic treatment, complicating infection management and treatment options.[ 3] Resistance arises through spontaneous mutation, horizontal gene transfer, and increased selective pressure from antibiotic overuse, both in medicine and agriculture, which accelerates resistance development.[ 6]
The burden of AMR is immense, with nearly 5 million annual deaths associated with resistant infections.[ 7] Infections from AMR microbes are more challenging to treat and often require costly alternative therapies that may have more severe side effects.[ 8] Preventive measures, such as using narrow-spectrum antibiotics and improving hygiene practices, aim to reduce the spread of resistance.[ 9]
Leave a Comment
Related Posts





/cloudfront-us-east-2.images.arcpublishing.com/reuters/UF3LTCUCNJKBHCQTIPTLHWYOSM.jpg)









/cdn.vox-cdn.com/uploads/chorus_asset/file/25008888/DSCF3714.jpg)



